Multidisciplinary Team for Type 2 Diabetes Care
- Good Country Physio

- 1 day ago
- 6 min read
Managing Type 2 Diabetes (T2DM) isn’t a single person job. It typically requires a team. That is why there is a heavy multidisciplinary aspect for Type 2 Diabetes care and management.
A multidisciplinary team is a group of health professionals who collaborate to provide optimal care and improve patient outcomes. In the instance of T2DM, multiple health professionals come into play. This includes:
Podiatrists
Dietitians
Pharmacists
Let’s have a look at what these health professionals do, and how they can help in the prevention or management of T2DM. As well as highlighting the impact exercise has on other forms of care.
Podiatrists/Footcare
What do podiatrists do for people with Type 2 diabetes?
Preventing and managing foot complications
Pressure management through footwear advice
Reduce the risk of serious complications
Education
People with Type 2 Diabetes are typically at a higher risk of experiencing:
Peripheral neuropathy – reduced sensation
Poor circulation – slower healing
This occurs as long term high blood sugar levels can cause damage to both the nerves and blood vessels within the foot. This results in nerves not being able to send signals to the foot and less oxygen and nutrients reaching the tissues. Overall, leading to,
Numbness, tingling and reduced sensation
Slow wound healing and tissue breakdown

Both of these factors contribute to foot ulcers and infections as individuals with T2DM are less likely to feel cuts, blisters and other open wound injures, which take longer to heal. High blood sugar also weakens the immune system which makes it harder for people with T2DM to fight infections that may arise from foot ulcers. This is why people may require amputations.
How can exercise help?
Whilst exercise cannot reverse foot damage caused by T2DM, exercise plays a role in slowing the progression of further complications. This can be broken down into the factors below.
Exercise can help with sensation
As mentioned previously, exercise helps control blood glucose levels. This has an effect on reducing nerve damage that causes sensations changes within the foot.
Furthermore, exercise supports nerve health through improving blood flow.
Exercise improves circulation
Exercise increases blood flow
When muscles contract, they push blood toward the heart, and this keeps repeating.
This increases blood flow from the feet, improving oxygen delivery and removing waste products.
What should you look out for?
Research shows that the warning signs are typically missed, which is why it is so important to check your feet daily, and book in for yearly foot checks with your local podiatrist. Here’s what to look out for.
Ulcers
Bunions
Ingrown toenails
Dry or cracked skin
Tingling, burning or pain
A sore that won’t heal
Skin discoloration
Swelling
Foot odour

Dietitians/Food
Dietitians play an extremely important role within the management of Type 2 Diabetes. Dietitians use evidence-based nutrition strategies to help prevent complications that arise from diabetes.
Studies highlight that working with a dietitian can significantly reduce average blood sugar levels, improve energy and weight stability. However, dietitian advice is not a “one size fits all” proforma. Many factors including, age, stress, activity levels and medication can influence an individual’s diabetes journey. Which is why it is so important for people to seek individual advice.
What can dietitians do?
Glycaemic index awareness - choosing carbohydrates that release energy gradually
Meal timing strategies - timed with insulin and medication
Smart food pairings - to allow for slower glucose absorption
Managing enjoyment food - allowing for occasional treats, favourite foods and working around social events
How do food and exercise interact?
Food and exercise go hand in hand, and they can have major effects on blood sugar levels in people with Type 2 Diabetes. This is because…
Food = controls how much glucose (sugar) enters the bloodstream
Exercise = controls how much glucose (sugar) is removed from the blood stream
Why is this important?
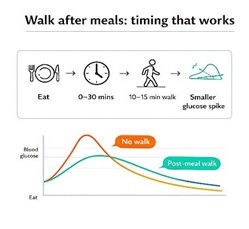
Incorporating light exercise 30-90 minutes after eating a meal, can have major beneficial effects. This is typically referred to as postprandial exercise. Studies completed in 2022 highlight that even a 2-minute walk after eating reduces blood sugar spikes.
In people with type 2 diabetes, blood glucose levels spike higher and last longer than people without diabetes
When you exercise after eating the muscles use glucose immediately for energy, meaning whilst sugar is entering the bloodstream, the muscles are taking it out and using it.
This causes a smaller spike as seen in the picture.
Possible Food Swaps
Whole milk to Skim milk
Cereal to Granola
Chips to Nuts
Butter – margarine
White bread – wholemeal
Milk chocolate to dark chocolate
Pharmacists/Medication
Pharmacists play a key role in the management of Type 2 Diabetes. This is typically through,
Medication
Blood glucose monitoring
Identifying side effects and interactions
Education
Medications are typically used when other points of contact have not worked. General Practitioners will suggest changing lifestyle factors such and exercise and food before oral medication. People may need insulin, if oral medication does not change their symptoms
How can exercise change medication needs?
As discussed previously, exercise helps
Improve the effectiveness of insulin
Increase muscle glucose uptake
Increase muscle mass
Over time, this means the body may not need as much help from external sources such as medication to manage blood sugar levels. Therefore, pharmacists may need to review medication, reduce dosages and adjust the timing of medications to fit your exercise program.
Exercise and Medication side effects
It is very important to talk to your pharmacist before making any major changes to exercise. Some medications such as insulin, metformin and other diabetes specific medications can have effects on exercise. Such as,
Fatigue
Dizziness
Reduced exercise tolerance
This is typically due to risk of hypoglycaemia. Hypoglycaemia is when blood sugar levels become too low. In people with type 2 diabetes the aim is to reduce blood sugar levels typically with exercise and medication. However, when blood sugar levels are too low, the patient can experience the symptoms seen above. Which is why it’s so important to liaise with your pharmacist, GP and/or diabetes educator about exercise and medication.

Diabetes Nurse Educator
What is a diabetes nurse educator?
A diabetes educator is a health professional who is an expert in the field of diabetes education and management. A diabetes educator can be the first health professional you liaise with if you want more diabetes specific information or help with management.
How can they help?
They can give advice, answer questions and help with your cycle of care
Teach you about diabetes
Help you monitor and manage blood glucose levels
Support lifestyle changes
Advice on how to use your medication
Inform you about other health problems you may be at risk of
What is a cycle of care?
Diabetes is an everchanging condition, that requires daily self-management to reduce the risk of short- and long-term complications. In order to reduce the risk of these complications an annual cycle of care is used as a checklist that is designed to measure diabetic control. It is an ongoing, continuous process, to keep people as healthy as possible.
What does it involve?
Your cycle of care involves regular checkups and reviews including,
HbA1c
Helps evaluate whether diabetes is well under control
Blood pressure
Having high blood pressure can increase the risk of stroke, kidney disease and heart disease
Cholesterol
Cholesterol is a type of fat in the blood. Having high cholesterol in the blood increases your risk of heart disease and stroke.
Eye assessment
Diabetes can cause eye complications that can lead to blindness if left unchecked
Foot assessment
Diabetes can damage the blood vessels and nerves within your feet, leading to reduced circulation and sensation changes
Kidney health
Diabetes causes an increased risk of kidney damage, as high blood glucose levels damages blood vessels and filters within the kidneys
This could lead to reduced function of the kidneys and potentially kidney failure

The multidisciplinary team is there to support people with diabetes. There overall goal is to help with daily management with the intent to make it easier and less overwhelming.
Helpful resources
Your healthcare team - https://www.diabetesaustralia.com.au/managing-diabetes/healthcare-team/
Diabetes and foot care - https://www.diabetesaustralia.com.au/living-with-diabetes/preventing-complications/foot-care/
Benefits of a 2 minute walk after exercise - https://edition.cnn.com/2022/09/02/health/walking-blood-sugar-study-wellness/index.html
Type 2 Diabetes and Medications - https://www.ndss.com.au/living-with-diabetes/management-and-care/medications/medicines-for-diabetes/
Diabetes Educator - https://www.diabetesaustralia.com.au/managing-diabetes/annual-cycle-of-care/
Taylah Searle & Kassidee Sayers
4th Year Bachelor of Physiotherapy (Honours)Adelaide University
Currently completing Health Promotion placement at Good Country Physiotherapy Naracoorte, supervised by Angela Willsmore.
Note: This information is of a general nature only and should not be substituted for medical advice or used to alter medical therapy. It does not replace consultations with qualified healthcare professionals to meet your individual medical needs.


Comments